chanawit / Dollar Photo Club
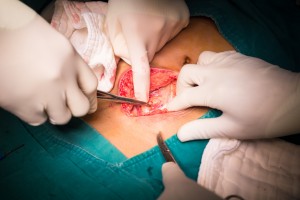
The common belief is that, if your appendix becomes inflamed and infected, it needs to come out now. As in like “emergency surgery” now.
It’s one of those situations where you would never think about doing a randomized study on it because it would be withholding life-saving medical treatment from those in the placebo group. Kind of like surgery to remove a tumor. Or like a clinical study to see if parachutes really do save lives.
It takes some forward thinking individuals to really challenge the status quo, and even once it has been challenged, it still takes years or sometimes decades before real change occurs. A perfect current example is arthroscopic knee surgery to go in and “clean out” the knee. Surgeons all thought it was a requirement to go in and clean everything out. At least until the VA did a placebo-controlled study on arthroscopic surgery of the knee and found that, after a year, there was no difference in the patients who had surgery and the patients who only thought they had surgery.
Years later, surgeons still refuse to change behaviors despite the strong evidence that they are not actually helping knee pain patients.
Dogma rules.
Back to your appendix. It has only been recently that scientists have determined that your appendix really does have a use. For pretty much ever, science believed that the appendix was a vestigial organ — and organ that we may have needed a million years ago but don’t need today. It is believed that the appendix basically acts as a storage organ for bacteria to repopulate the gut after a severe infection in the gut such as cholera or Salmonella.
Sounds like a good idea to me, especially considering how important the bacteria in your gut are for health.
This was, of course, before the time of heavy duty antibiotics that can pretty much wipe the slate of your gut clean of all the bacteria that we’d like to have growing there, leaving other bacteria that we do not want growing to thrive, like the Clostridia family (think C. diff infections).
But when your appendix becomes infected and inflamed, what options do you have? As mentioned, surgery is generally considered the only option. But, just like so many other procedures that we take for granted are the best options, the answer is not always so clear. In this particular study, researchers looked at what happened when uncomplicated acute appendicitis was treated with antibiotics instead of surgery in 530 patients with CT-confirmed appendicitis (this is not the time to bring up ultrasound versus radiation overload CT-scanning…). For reference, uncomplicated appendicitis refers to an infection of the appendix that does not involve a perforation or an abscess formation.
Patients were given either antibiotics (intravenous ertapenem @ 1 g/day for 3 days followed by 7 days of oral levofloxacin @ 500 mg once daily and metronidazole @ 500 mg 3 times per day) or had surgery to remove the appendix. Here’s what happened:
- In the antibiotic group, 70 patients (27.3%) still ended up undergoing an appendectomy within 1 year. The remaining 186 (72.7%) avoided surgery.
- Of the 70 patients in the antibiotic group who ended up having surgery, 58 (82.9%) had uncomplicated appendicitis, 7 (10.0%) had complicated acute appendicitis and 5 (7.1%) did not have appendicitis but received appendectomy for suspected recurrence.
- There were no abscesses or other major complications associated with having a delayed appendectomy.
In other words, darn near 3/4 of these patients did NOT need to have an organ they were born with removed. Granted, the rather large doses of antibiotics given in the non-surgical group presents its own set of problems, but when balanced against the removal of an organ that we don’t know all that much about, but deals with bacterial flora in the gut, I think I’d take the antibiotics. Besides–you’re still going to get a hefty antibiotic dosing if you had surgery anyway, so why not try to save the organ?
What’s nice to know is that, out of 256 patients who received the antibiotics, only 7 (2.7%) later presented with a more complicated infection. Those are pretty good odds.
One other thing to consider. What would have happened if the antibiotic group were followed up with high dose probiotics to combat the ill effects of the antibiotics? Personally, I think there’s a very large possibility that the 27.3% of patients who still needed surgery would be a much smaller group.
